Facing COVID Fatigue: Life on the NHS Frontlines
Dive into the emotional realities faced by NHS staff on the frontlines during COVID-19, revealing the fatigue, challenges, and coping mechanisms that define their experiences.
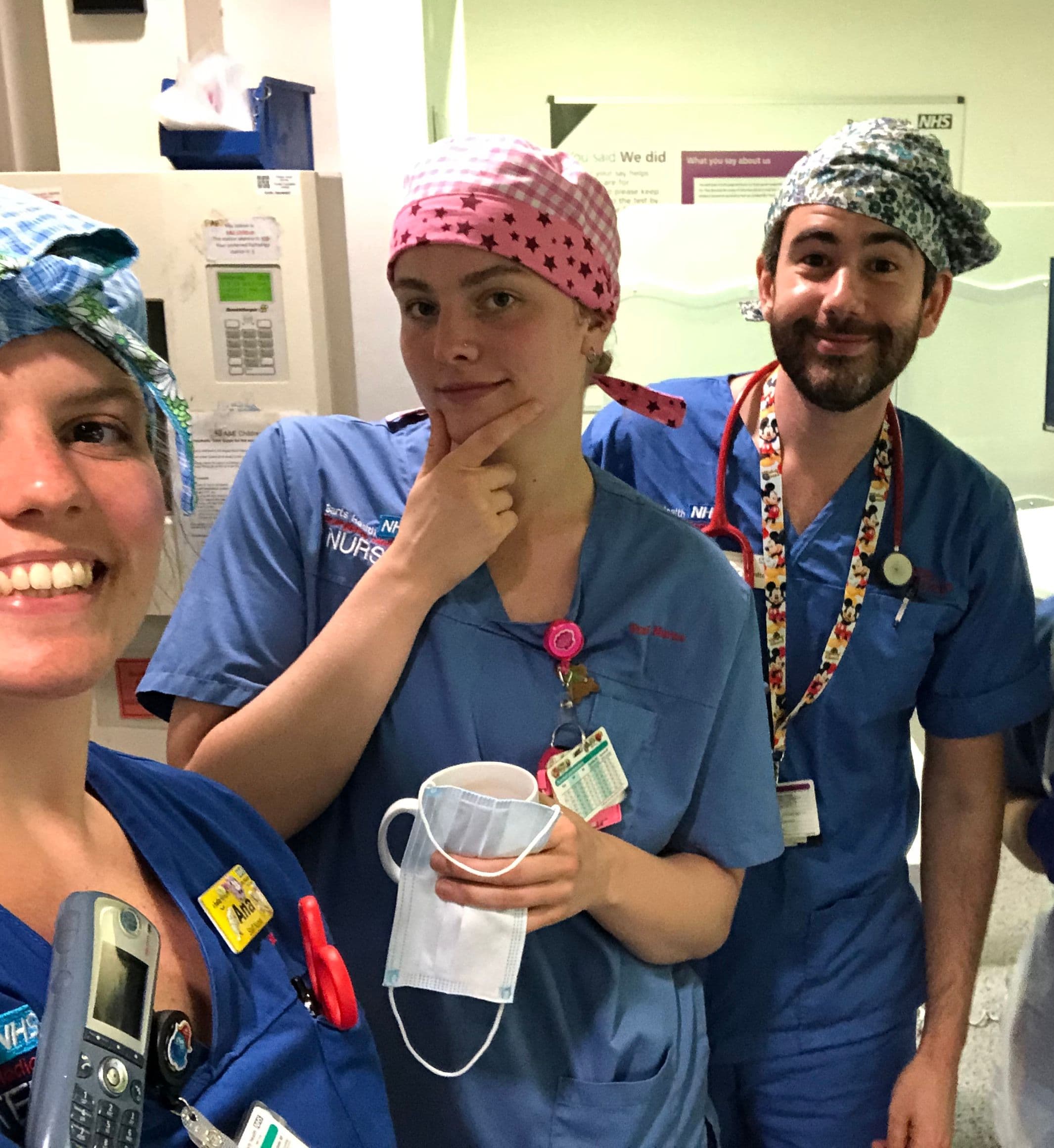
Dive into the emotional realities faced by NHS staff on the frontlines during COVID-19, revealing the fatigue, challenges, and coping mechanisms that define their experiences.

Working in healthcare is never easy; but working through the Covid-19 pandemic takes all the usual stresses, strains and anxieties and amplifies them by a factor of ten.
The mood in my Accident & Emergency (A&E) department at an east London hospital is highly emotional. Apart from the heavy case load, we are also affected by the uncertainty of COVID-19. This includes having to defer those personal plans and hopes that can help to keep you going in the ever-strained atmosphere of a hospital emergency department.
Recently, a nurse I’d never met before broke down in our changing room because she had had to cancel a much-needed holiday break. “I really needed this holiday”, she said. “I’ve been saving up for a whole year”. Our most-used methods of coping have been stripped from us and we’re having to find different ways to manage.
The fear of spreading the virus to others is particularly acute for healthcare workers. A friend texted me to say that she’s terrified that she could cause the death of family members. She’s constantly disinfecting surfaces and cleaning. And she’s not the only one. I’m not looking forward to the next water bill, given the amount of time I spend washing my clothes and showering. As medical staff we feel that we should be constantly working, permanently manning the barricades. A colleague told me she feels “helpless” on her days off: she wants to go back to the hospital to help out.
Much has been written about night shift anxiety; the sense of isolation and disconnect from wider society that comes with working nights. In the current emergency, these feelings are more acute, and they are not limited to night work. Healthcare workers are living different lives to most people.
It is like being in a different time zone or being a ghost in the normal world we inhabited until just recently. The world has turned into a Rorschach test and we’re seeing and experiencing things differently to everybody else. Nevertheless, the generosity of others is extremely precious in these times – the public demonstrations of support, such as the nightly applause and pot-banging in London, often move me to tears.
We know that, as healthcare professionals, we’ll have to make difficult decisions that we haven’t had to make before. We have to break terrible news to a patient without any of their family being present or make agonising calls on access to ventilators. As a result, we run the risk of ‘moral injury’ – the psychological damage from being forced to violate one’s moral values.
This article is part of Global Geneva’s regular coverage of personal stories about the coronavirus crisis. A reminder: we make our content free worldwide in the public interest. If you like what we do, please support us.

The decisions are similar to those faced by soldiers or aid workers in war zones. There are likely to be cases of post-traumatic stress when this is all over. Recently, faced with a Covid-19 patient scared of dying, I could only smile behind my facemask and offer a gloved hand to calm her down: giving her a hug was not an option.
What can we do to keep ourselves functioning and healthy in these trying times? Many of the normal tricks used to confront the usual anxieties associated with healthcare work can’t be applied to Covid-related anxiety. A clinical psychologist I know says that teaching your mind not to become preoccupied with “wandering” thoughts is important.
She recommends making a concerted effort not to focus on the negatives, absences and perceived service failings; not to let your mind drift to the things you aren’t doing, the social bonds you aren’t able to maintain, the news and information you aren’t keeping up with. Instead, try to focus on what you are doing, which is, as she and many others insist, amazing. She has a simple message: “You are doing enough. You are enough.”
At work, finding new methods of coping has become key. Ensuring we take time to ask each other if we are okay is crucial. With expressions obscured by masks, it’s become a vital new healthcare skill to be able to tell what emotions people are going through solely by looking at their eyes. Checking up on each other has become really important, and I’m particularly enjoying the new ways of being affectionate at work – elbow tap here, toe tap there.
With the help of friends and colleagues, I’ve added a few other techniques to the toolkit I’m using to help deal with Covid-19 anxiety.
Firstly, I’ve bought an alarm clock so that when I go to sleep, I can leave my phone in a different room. That way I’m more disconnected from the world when I’m resting, and less tempted to catch up on things if I wake up in the middle of the night. And when I do get up, I don’t open my eyes to a bombardment of push-up notifications, emails and frenzied messages.
Secondly, I make sure I do some form of exercise once a day – even if this means following a pre-recorded boxing class via a choppy video stream.
And finally, I make sure to properly relax during my time off by pencilling in some time for just sprawling on the sofa and watching rubbish TV. Just make sure that the new series doesn’t have a pandemic-related sub-plot before you get stuck into it.
This article (see link) was originally published on the ‘Don’t forget the bubbles’ Paediatric Medical Educational platform.
Ana Waddington is a senior nurse in A&E at a major trauma hospital in London. Born in Chile to an English father and Spanish mother, she has lived in other countries notably Italy, Portugal, Switzerland, Morocco and the UK. After taking a history degree at SOAS, she worked in the charity sector and then trained as a nurse. She volunteers with NGO’s supporting refugees and has set up an organisation – Yourstance – to help young people affected by serious youth violence in London. Ana also writes for ‘Don’t Forget the Bubbles’, a paediatric medical education platform.

Coronavirus Stories: Lessons from the roller coaster life of an Italian ICU nurse
Pangolins and pandemics: digging for the roots of COVID-19
COVID-19 and climate change: the planet’s twin crises
Coronavirus Stories: My Verbier Covid-19 Experience
Coronavirus Stories: When uncomfortable becomes comfortable
Coronavirus: Community participation and credible information: the core of any serious response
COVID-19: Is the Swiss government engaged in false news and not doing its job?
Impact investing and SDGs in the COVID-19 era: maths matters more than opinion